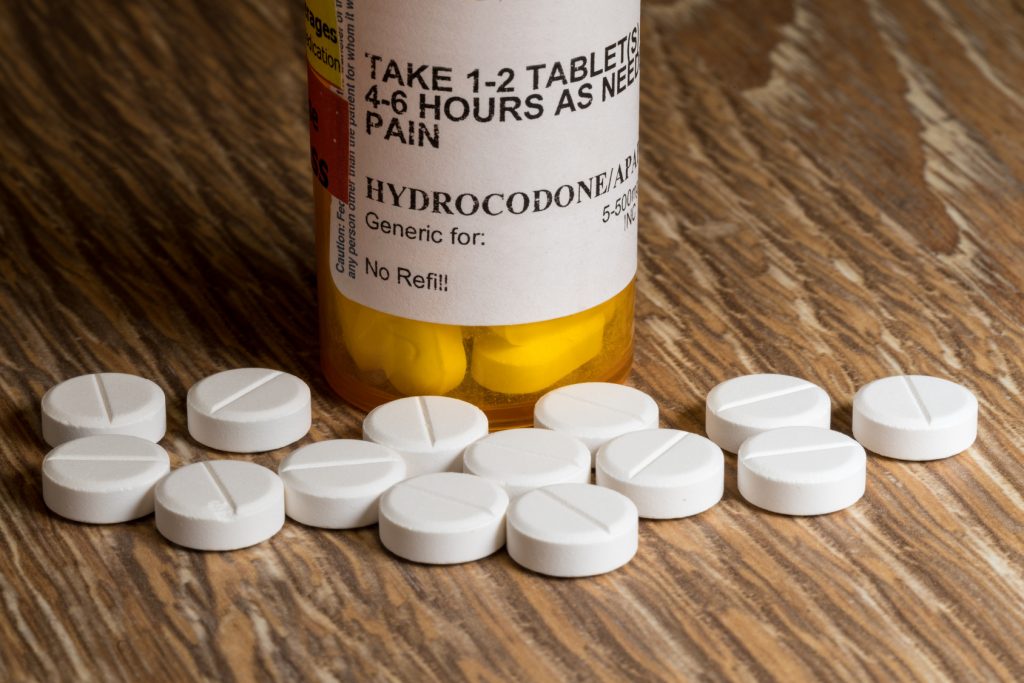
opioids
TagHospitals Sue Drug Makers Over Cost of Treating Opioid Addiction
In recent weeks, hundreds of hospitals have joined the fight against the opioid epidemic by filing suits against the highly addictive drug’s makers and distributors.
Landmark Decision Holds Drug Maker Responsible In Opioid Crisis
An estimated 130+ people die every day from opioid-related drug overdoses, and now a landmark decision in Oklahoma is holding one drug maker responsible.
Surgeons’ Opioid-Prescribing Habits are Dangerous, Persistent
As the opioid crisis escalated into an epidemic across the U.S., thousands of surgeons continued to hand out far more pills than needed.
Oklahoma’s ‘Precedent-Setting’ Suit Puts Opioid Drugmakers On Trial
All eyes were on Oklahoma last week, when the first case in a flood of litigation against opioid drug manufacturers began Tuesday.
Federal Task Force Pushes PT as an Alternative to Opioids
A report released this week by an inter-agency task force highlights the benefits of physical therapy and other modalities in combatting the opioid crisis.
New Opioid Approved by FDA, Mere Days After Trump Signs Opioid Bill
On October 24th, President Trump signed a package of bills designed to confront and combat the nation’s opioid epidemic. On November 2nd, the FDA approved Dsuvia.
How Alternatives Such as CBD Oil Make an Impact on the Opioid Epidemic
As the opioid epidemic continues to wreak havoc on the United States, we take a look at the viability of cannabidiol as an alternative.
Majority of Patients Expect Opioids After Surgery
Despite campaigns by the therapy community, and the government, to loosen the grip of opioids in the U.S., patients still expect them after surgery.
PT Supported Opioid Bill Ready for President’s Signature
Landmark legislation to fight the opioid epidemic, supported by the APTA, is headed to the President’s desk to be signed into law.
Stark Facts About Opioid Misuse in the U.S.
Physical therapy is a viable alternative to opioid use. Yet, nearly 48,000 Americans died due to opioid related overdoses last year.