Advanced Practice
CategoryThree Ways to Celebrate PA Week
Here are three ways to celebrate PAs, while also raising awareness of the profession’s significant impacts on healthcare, from October 6th through 12th.
Drama Series with NP Protagonist Heads to Netflix
A new romance drama series with a nurse practitioner at its heart is headed to the small screen, bringing exposure to the NP profession through entertainment.
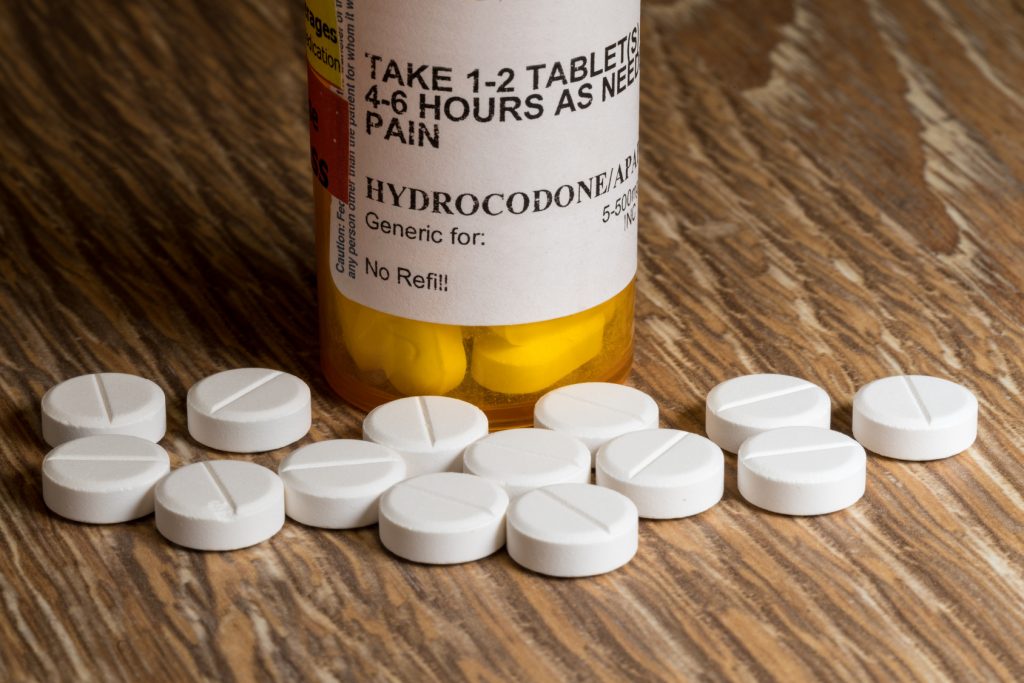
New Legislation Arms Advanced Practitioners in the Fight Against Opioids
More than 115 Americans die every day from opioid-related causes. The SUPPORT for Patients and Communities Act, which passed in the House last week, aims to stop that.
Steal this Recruiter’s Tips to Land the Perfect Job
Seeking a competitive advantage to help you land your perfect job? Look no further than this advice from a clinician who has been involved in hiring.
Using Medical Survey Panels to Grow Your Clinical Income
Explore the benefits, as well as the downsides, of participating in medical market research survey panels as a way to supplement your income.
44 Million Reasons to Expand Scope of Practice
13% of the population of the U.S. now lives in a county that is experiencing a primary care physician shortage. Advanced practitioners could very well be the answer.
Tired of Peer-to-Peer Phone Calls with the Insurance Company?
There are techniques and processes you can develop to make your life easier when dealing with the oft-labeled “bureaucratic nightmare” of insurance companies.
Advanced Practitioners Contribute Greatly to Cancer Care
The first large-scale study of NPs and PAs in oncology shows that not only are advanced practitioners directly involved in patient care, but they also like their jobs.
Best Non-Clinical Side Hustles Any Clinician Can Start – Part 2
Part two of this series explores the non-clinical options of landing clinical speaking opportunities or joining paid medical market research panels.
Kim’s Blog: Stand Up and Support Patients’ Wishes
What effort does it take to support a patient’s wishes? It’s not merely documenting them, but putting the wheels into motion to do, or to NOT do things.