Health Care Information on the Cloud—or Anywhere. Is It Really Safe?
Why is it even on the cloud? If it is unsafe, can it be made safe? What can I, as a business owner or business manager, do about it?
Nurses: What Tips & Tricks Do You Have to Share?
Whether you’re a new grad or about to retire, we’re willing to bet you have tips and tricks to share with your fellow nurses, and we want to hear them.
Thriving as a Nurse in Underserved Communities
What’s it like working as a nurse in an underserved community? What skills and qualities should nurses have in order to succeed in this area?
New Report Says Primary Care Salaries Jumped by $22k in 2016
Signing bonuses also increased from an average of $19,714 in 2015 to $27,799 in 2016.
Recovering From Physician Burnout
by Lori Corley
My name is Lori Corley and I am recovering from physician burnout. There is a lot of discussion and education about physician burnout recently, but this was not always the case. Physician burnout is that point where you love and ha…
Does a Doctorate of Nursing Practice Make a Difference in Patient Care?
The question of whether the DNP impacts patient care has arisen among many NPs who hold those DNPs.
New AMA Policy Opposes Autonomous State PA Boards
At the annual meeting of the AMA, held June 9-14, 2017, delegates passed a resolution opposing autonomous state PA boards.
Top 10 U.S. Biopharma Clusters
All 10 regions ranked have significant assets that make them attractive to biopharma researchers, executives, and investors.
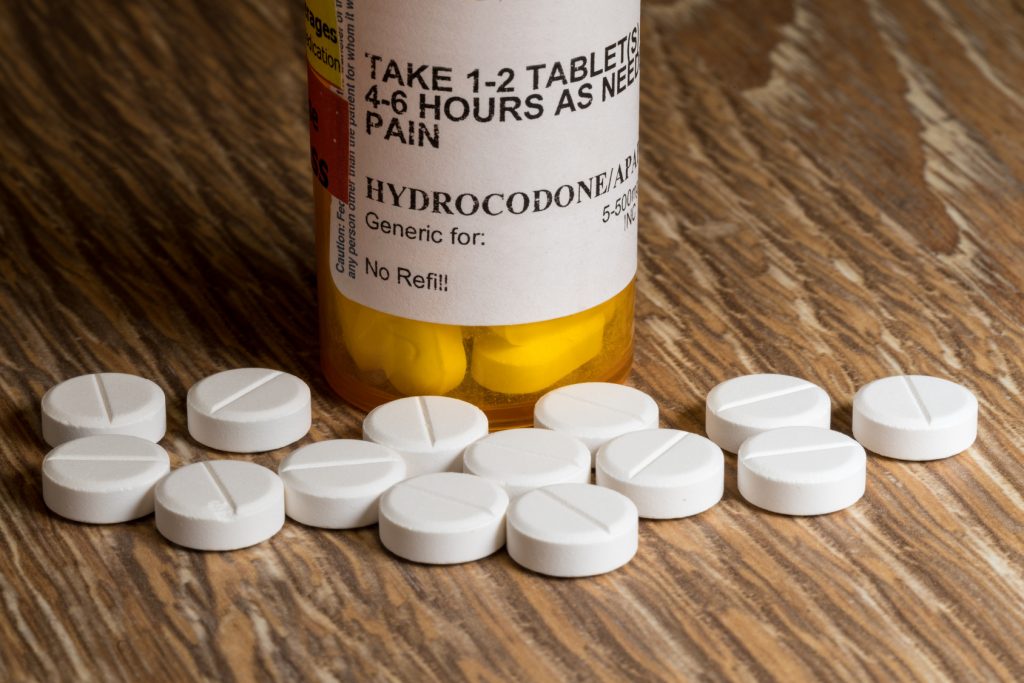
Are Pharmaceutical Companies to Blame for the Opioid Epidemic?
Recent lawsuits are asking courts whether the current crisis is comparable to the one over tobacco in the ’90s.
App Helps Users Find Ear-Friendly Places
Users of the iHEARu app help one another locate quieter spaces and hearing technology access through sound ratings and reviews.